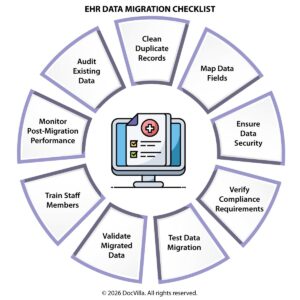
EHR Data Migration Checklist: A Complete Guide for Medical Practices Switching Systems
Switching Electronic Health Record (EHR) systems is one of the most complex and high-risk transitions a medical practice can undertake. While the decision to move to a new EHR or integrated practice management platform is often driven by the need for better workflows, improved usability, or enhanced features, the process of migrating data from one system to another requires careful planning and execution. Patient records contain critical clinical, financial, and operational information that must be transferred accurately to ensure continuity of care. Any errors during migration can disrupt workflows, delay patient care, and create compliance risks. For this reason, medical practices must approach EHR data migration with a structured strategy that minimizes risk and ensures data integrity. A well-defined migration checklist helps practices prepare for each stage of the process, from initial planning and data mapping to testing, validation, and post-migration optimization. Practices that follow a comprehensive migration plan can avoid common pitfalls such as data loss, mismatched records, and workflow disruptions. In addition, selecting a modern, cloud-based EHR and practice management platform can simplify migration by offering better tools for data import, integration, and ongoing system updates. This guide provides a detailed EHR data migration checklist designed to help medical practices transition smoothly to a new system while maintaining operational efficiency and patient care quality. … Read More











































